Articles & Resources - Iliotibial Band Friction Syndrome
Iliotibial band friction syndrome is a common source of knee pain that is often described as a “stabbing pain” at the outside of the knee. It is most common in activities that require repetitive bending and straightening (flexion and extension) of the knee such as running and cycling and is typically an “overuse” type of injury as opposed to an injury that results from trauma.
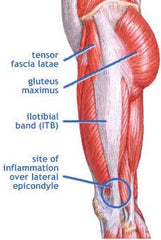
Anatomy and Function
The IT Band is a long, wide and relatively thick sheet of connective tissue that originates from the iliac crest of the pelvis and fascial components of the gluteus maximus, gluteus medius and smaller tensor fascia latae muscles. It runs down the side of the thigh and inserts into the lower outside part of the thigh bone (lateral femoral condyle) and the top of the fibula with some fibers attaching on the lateral side of the kneecap. Under normal circumstances the IT Band slides back and forth over the lateral femoral condyle as the knee flexes and extends. Other than wreak havoc with many people, it does have a purpose: it works as a lateral stabilizer of the hip, assists in abduction of the hip and helps control adduction of the hip; it also plays a role in lateral stability of the knee.
Symptoms
Pain from the IT Band usually presents itself as a sharp, stabbing pain at the side of the knee during and sometimes after activity. Same-sided hip soreness may also be present. As is the case for any injury with pain lasting more than a few days, always seek the advice of a medical professional for accurate diagnosis.
Causes
As with most injuries associated with overuse, training errors are probably the single greatest cause of ITBFS. When a repetitive activity or workload is greater than the tolerance level of a structure or tissue, inflammation and pain will result. The most common training errors relate to the frequency, duration and/or the intensity of an activity or training program; too much too soon in the absence of proper recovery puts the IT Band at risk for injury.
Tight and weak hip and thigh musculature can stress the IT Band due to the result of excessive femoral adduction and internal rotation of the thigh. Muscle fatigue, poor run or cycling technique, leg length discrepancies, and excessive foot pronation also increase the stress along the iliotibial band. Other risk factors include improper equipment fit such as bike fit or worn running shoes. Myofascial restrictions or scar tissue from a prior injury to the hip or thigh and/or trigger points in the hip or lateral thigh muscles can also contribute to IT Band pain.
Treatment and Prevention
As with any musculoskeletal or soft tissue injury, effective treatment starts with proper diagnosis. Treatment of ITBFS begins with activity modification or total rest and ice. Ice is an effective, inexpensive natural anti-inflammatory and analgesic and can be used whenever there is pain, no matter if it’s a day or few months after the injury. If pain continues for more than a few of days, consult a medical professional.
Once cleared to resume activity or training, analyze your program and identify and fix any training errors that might have contributed to your problem. Replace worn shoes and consider a replacement insole in all of your shoes for optimal support and shock absorption. Review your strength and conditioning program and be sure to include hip and core strengthening, especially of the gluteus medius, maximus and external rotators. Do not start training where you left off but at 25% – 50% of your usual program and increase 10% or so a week from there or as instructed by your physical therapist, doctor or coach.
Warm up and stretch well. The IT Band itself will not stretch so it is most effective to stretch the surrounding gluteal, quadriceps and hamstring muscles. Soft tissue mobilization should also be considered for treatment and can be accomplished through manual techniques or foam roller. The foam roller basically serves as a deep massage to the outside of the thigh and can be very uncomfortable at first so it should be utilized with care: start with a minute and work up to 3 – 4 minutes at a time rolling up and down the outside of your thigh.
Looking at the causes you might easily guess prevention. Appropriate preparation, proper equipment fit, technique and adequate recovery time (the PETR Principles©) are some of the best prevention measures and a must for anyone who regularly participates in any sport.
Preparation. The goal of preparation is to increase the bodies’ physiological tolerance so the demand of any particular sport or activity does not break it down to the point of injury. The better prepared the body is, the more resistant it is to stress and injury. Preparation includes appropriate warm up, flexibility, strength, endurance and balance training. Flexibility and strength specific to the Iliotibial Band include the hip, thigh and calf muscles because these help control and reduce excessive adduction and internal rotation of the thigh (femur) and internal rotation of the shin (tibia).
Equipment specific to the ITB includes footwear and bike fit. Movement of the foot influences movement at the knee and hip so daily and sport specific footwear is important for appropriate support, shock absorption and fit. For example, if you’re a runner, wear a shoe designed for jogging, not tennis or basketball; if you’re on your feet all day be sure to wear a shoe that offers good support and cushion.
Cycling involves repetitive movement of the legs through a relatively large range of motion, against a resistance, and takes place while sitting on a fixed seat leaning forward. This posture creates a specific geometry between the body and the bike and if not fit correctly can cause excessive stress on the knees, hips and back. For example an internally rotated cleat position and a seat that’s too high or too far back can stress the IT Band. And if you use insoles or orthotics to prevent excessive pronation in your non-cycling shoes, then you may also benefit from a shim on your cycling shoes. When fit correctly, the bike can be optimized to produce the least amount of stress while maximizing force production and comfort.
Technique refers to movement patterns required to perform an activity or sport efficiently and successfully. Generally speaking, the better the technique, the less the risk is of injury and the more successful the result.
For example, inefficient running gait can contribute to excessive tension and friction on the IT Band. A quick fix can be cadence. Simply stated, cadence is the number of steps taken per unit of time, usually one minute. Beginner and less experienced runners tend to over-stride which produces more impact force and stress on the knees as well as the feet, hips and back. Runners with a higher cadence (~180 steps per minute and higher) have a shorter stride and a foot-strike that that is more beneath their hips. This improves efficiency and creates less impact forces than those with a lower cadence (~160 to 170 steps per minute). Proper technique is important and can be learned with any movement or sport.
Recovery must always be included in a training program to allow the body to heal and adapt. Adaptation is how the body develops strength and endurance and it is during rest and recovery the body repairs and regenerates. Recovery can include easy training days, complete days off and sleep. As the volume and intensity of the workouts increases, so do our sleep and recovery needs. Without adequate rest and sleep we lose fitness. Recovery is the key to getting stronger and faster. Strength is gained during recovery periods, not during the actual work out.
Bottom line: the principles of proper preparation, equipment, technique and recovery will help prevent overuse and potential injury to the IT Band.
Coaching
You may also want to consider a coach or trainer with in depth knowledge of your activity. Whether you are a recreational or professional athlete, no matter how serious you may or may not be about a particular sport, a little knowledge can go a long way in not only improving performance but in preventing injury.
Conclusion
Although IT Band Friction Syndrome can be painful and debilitating, it is also very treatable and can be avoided. The trick is proper diagnosis and treatment. Proper preparation, equipment, technique, and recovery techniques are important and should be a part of every active persons program.
Partial list of references
Asplund, Chad MD, CPT; COL St Pierre, Patrick MD, The Physician and Sports Medicine - Knee Pain and Bicycling Fitting Concepts for Clinicians VOL 32 - NO. 4 - APRIL 2004
Ellis R, Hing W, Reid D. Iliotibial band friction syndrome--a systematic review. Man Ther. Aug 2007;12(3):200-8.
Hamill J, Miller R, Noehren B, Davis I. A prospective study of iliotibial band strain in runners. Clin Biomech (Bristol, Avon). Jun 24 2008;
Messier, S.P., Edwards, D.G., Martin, D.F., Lowery, R.B., Cannon, D.W., James, M.K., Walton, W.C., Read, H.M., Hunter, D.M., 1995. Etiology of iliotibial band friction syndrome in distance runners. Medicine and Science in Sports and Exercise 27, 951–960.
Miller, R.H., Lowry, J.L., Meardon, S.A., Gillette, J.C., 2007. Lower extremity mechanics of iliotibial band syndrome during an exhaustive run. Gait and Posture 26, 407–413.
Noble, C.A., 1980. Iliotibial band friction syndrome in runners. American Journal of Sports Medicine 8, 232–234.
Noehren, B., Davis, I.S., Hamill, J., 2007. Prospective study of the biomechanical factors associated with iliotibial band syndrome. Clinical Biomechanics 22, 951–956.
Taunton, J.E., Ryan, M.B., Clement, D.B., McKenzie, D.C., Lloyd-
Smith, D.R., Zumbo, B.D., 2002. A retrospective case–control analysis of 2002 running injuries. British Journal of Sports Medicine 36 (2), 95– 101.
- Choosing a selection results in a full page refresh.